Physiotherapy Treatments
Our approach to physiotherapy:
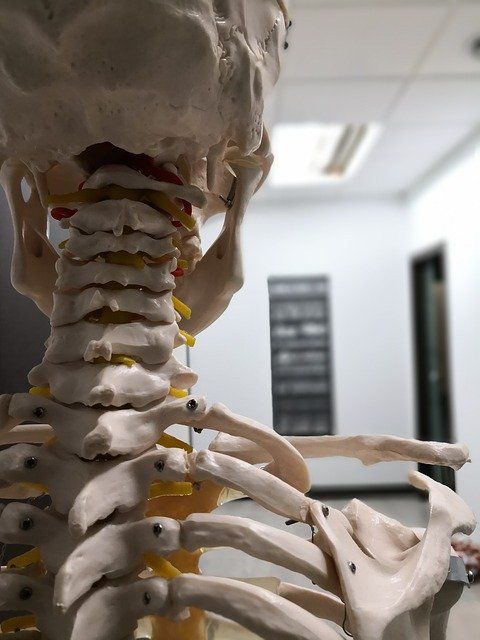
More often than not, injuries cause limited ranges of movement (ROM). This in turn will affect patients’ daily functions such as bending down, walking, moving arms and legs free of pain. In order to treat the condition, movement must be restored. This is why focusing on the provision of a movement-enabled
physiotherapy to achieve the treatment goal of restoring function whilst strengthening associated muscle groups to minimise the risk of future injury.
Human body is designed intelligently to initiate self-healing, once a full ROM has been made possible. A combination of manual therapy & exercise therapy can help correct limitations allowing a timely rehabilitation & recovery so that you can go back to your routine activities.
Injuries treated:
Whiplash associated disorders/pain | Postural related pain & deformities | Sports injury | Headache | Lower back pain | repetitive strain injury | Sciatica | Arthritis | Carpal Tunnel Syndrome | Chronic pain syndrome | Dizziness, vertigo & imbalance | Wrist pain | Shoulder pain | Frozen shoulder | Tennis elbow | Golfers’ elbow | Military neck | Bursitis | Dancing injuries | Plantar Faciitis | Achilles Tendinopathy | Achilles Tendinitis | Osteoarthritis (OA) | Hip Osteoarthritis | Knee Osteoarthritis | Joint Osteoarthritis & MORE!
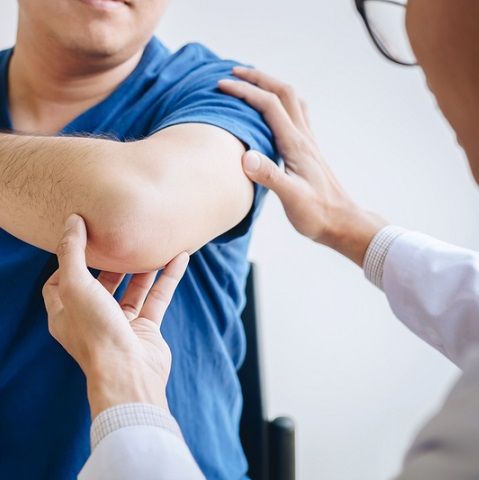
Physiotherapy
Choices include:
Assessment | 30min
Assess + Treat | 60min
Assess with Ultrasound | 30min
Assess + Treat | Home Visit | 60min
Treatments Include:
 Manual Therapy
Manual Therapy  Gait Analysis
Gait Analysis
 Manipulation (i.e. clicking)
Manipulation (i.e. clicking)  Standard Physiotherapy
Standard Physiotherapy
 Electrotherapy (Laser & TENS)
Electrotherapy (Laser & TENS)  Injection Therapy .
Injection Therapy .
 Soft-tissue Release
Soft-tissue Release  Acupuncture .
Acupuncture .
 Exercise Therapy
Exercise Therapy  Patient Education
Patient Education

Acupuncture
Stroke rehabilitation | Headache & Migraines | Menstrual cramps | Fibromyalgia | Myofascial pain | Osteoarthritis | Low back pain | Carpal tunnel syndrome | Difficulty breathing | Dental pain | Labour pain
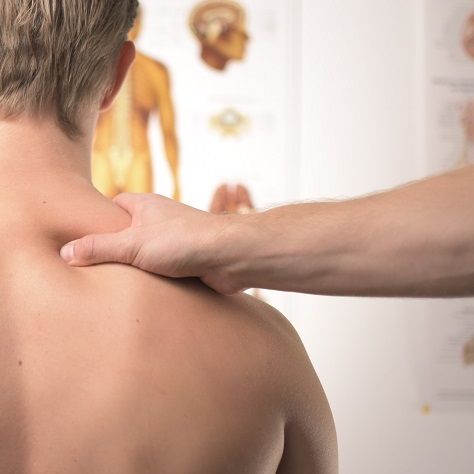
Massage
Deep tissue, full-body or sports injury massage are among some of the most popular massage therapy treatments we offer.